April 30, 2007 Update
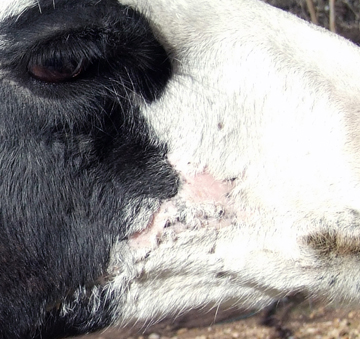
Glacier is healthy and has recovered completely from his rattlesnake bite on Sat April 15, 2000 except for a large hairless patch on his right cheek from which several narrow, hairless lines extend downward alongside and under his right jaw (see photo to the right). The patch does sunburn so we occasionally treat it with zinc oxide to keep it soft and prevent infection.
I continue to receive several queries a year from llama (and sometimes dog) owners about how to treat their animals' snakebites. Dr. Jensen is no longer at Texas A&M's Large Animal Medicine and Surgery clinic. His contact information for veterinarian referral calls may be found on the South Central Llama Association vet net page.
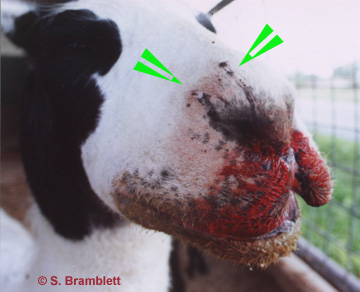
Day 2: Early Sunday morning we took Nova, our 17 mo old female llama, to be a companion to Glacier. He was walking in the pen when we arrived, and alternated walking with kushing for the 4 hours we stayed. He tried to drink, dipping his muzzle in the water bucket, but we couldn't detect swallowing because of the swollen neck. He would not eat. Karen Conyngham met us there and brought llama snakebite literature and helped support us, as well as Glacier.
Day 3: By Monday, Glacier's eyes were almost swollen shut and he stumbled about the pen. He did try to drink water, but was uninterested in food. I e-mailed several questions to Dr. Jensen at Texas A&M University's Veterinary School, Large Animal Clinic, and he replied quickly. We could expect to see maximum swelling at 48-72 hours. It was OK that he not eat for several days, if he had been in good condition before the snakebite (he was). Because rattlesnake bites can cause severe necrosis and permanent tissue damage, it is not uncommon for surgical debridement of necrotic tissue at some stage of recovery. I asked about Dr. Jensen about the feasibility of taking Glacier to A&M, but he felt the long, hot trip might be dangerous and that he was in good hands with Drs. Portie and Crossland.
Day 4: Eye swelling was reduced. He continued to receive tubed nutrients and I.V.s daily, and antibiotics every three days. Upper lip swelling decreased, but his lower lip remained grotesquely distended.
Day 5: Normal eyes; upper muzzle smaller; lower lip still badly swollen.
Day 7: ProBios was administered and Glacier ate some Muenster (extruded feed supplement).
Day 9: Reduced lip swelling; no defecation; not eating; vomited; frequent drinking.
Day 10 : Dr. Portie transfaunated Glacier with cow rumen via a tube. The antibiotics killed the normal rumen flora and fauna (protozoans and bacteria), resulting in an inability to digest food.
Day 11: Because he would not eat, we took him home to see if he would do so under more normal circumstances. He drank water for 40 minutes, but still did not eat. He would "sham" feed, taking bits of hay, then letting them fall out of his mouth.
Day 12: We returned Glacier to Dr. Portie's clinic. Dr. Jensen advised that Glacier probably had gastric ulcers from the necessary supportive treatment for snakebite (Banamine, oral drenches, and general stress) and recommended Omeprazole (Prilosec for humans) and diagnostic blood work (WBC and fibrinogen) to diagnose. Dr. Portie began Omeprazole treatment. Fibrinogen levels were normal, but it may be early ulcer development.
Days 14 and 15: Dr. Portie, after consulting Dr. Jensen, recommended that we take him to Texas A&M University's Veterinary School. We did so, arriving about 8:00pm. Dr. Jensen met us there and worked with Glacier until 11:00. During our visit the next morning, Dr. Jensen explained that nutrients and fluids would be infused via a jugular catheter suspended from a tether to rehydrate and feed him. He cleaned scabs from the right nostril and Glacier's breathing improved. Glacier now weighed 244 lb, having lost 35 lb. in two weeks. Because he was so dehydrated, they were unable to insert the catheter. He was given 5 liters of fluids I.V., Omeprazole, and a blood panel was run. He was urinating and defecating.
Day 16: Glacier's arched posturing and tooth grinding may indicate kidney pain. 5 more liters of fluids were administered. When checking on the llamas at 10:30pm, Claud found and killed a 4 ft rattlesnake only 20 ft from our four kushing llamas.
Day 17: He still was not eating or drinking. No normal digestive organisms were found in his rumen; his arched posturing and tooth grinding are also indicative of severe heartburn. Normal throat and nasal tissues were revealed by endoscopy. A rumenectomy was performed (a quarter-sized hole was made into the left side just behind the last rib; the rumen lining was sutured to the skin, and a plastic syringe sewn into the hole, through which electroytes were infused. A cap on the syringe kept contents from spilling out. Urinalysis results (BUN 54; Cr 4.6)
Day 19: Glacier ate a hay flake; not drinking water; urinating & defecating. Rumen pH 6.3 is too acidic. He was infused with a gallon of water (and pulverized goat chow) thru rumenostomy.
Day 20: Drinking water; ate hay; normal kidney function. A blood and electrolyte panel was run.
Days 22 and 23: He still had low rumen organism counts; low (acidic) pH; and still had no formed feces. He was "transfaunated" (transfer of fauna) with 0.75 gal of donor cow rumen. A&M has a cow with a permanent fistula (hole) in her side, closed with a removable "plug," from which rumen can be taken when needed.
Day 24: He began eating hay, Muenster, and drinking. A rectal exam showed formed feces. Day 25 (May 9): We took Glacier home today! The syringe was removed and we took him home with an open hole in his side through which rumen would slosh out, soiling his side. We had to clean it twice a day and use fly spray to keep maggots out of the wound. Dr. Jensen said it would heal closed in a month or two.


